Hygiene Solutions prime sales presentation for Deprox centres around a drop in C. difficile infections at Addenbrooke’s Hospital in 2009/2010. Here is the graph, which is presented in various colours in several successive PowerPoint slides.
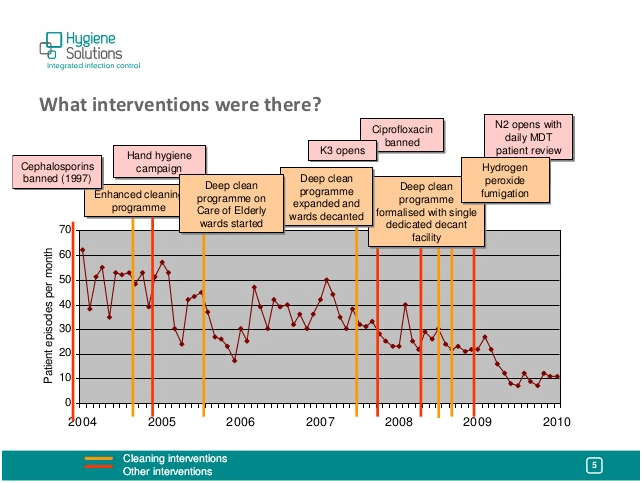
The point that their salesman labours is that there is a drop in C. difficile rates in 2009 coinciding with the introduction of hydrogen peroxide fumigation. None of the slides actually say that this was Deprox fumigation, which is very honest of Hygiene Solutions, because it wasn’t.
Given the much larger and unexplained variations in 2005 and 2006, the statistical significance of the short period shown after fumigation introduction is very dubious. Even worse, no allowance is made for the national trend, which should be subtracted from the local data if a local effect is to be demonstrated. Below is the national trend for the same period – In 2009, the number of C. difficile infections declined more rapidly than for any other year since records started. This would account for about half of the 2009 reduction shown on the graph above, which leaves the “data” very much smaller than the “noise”.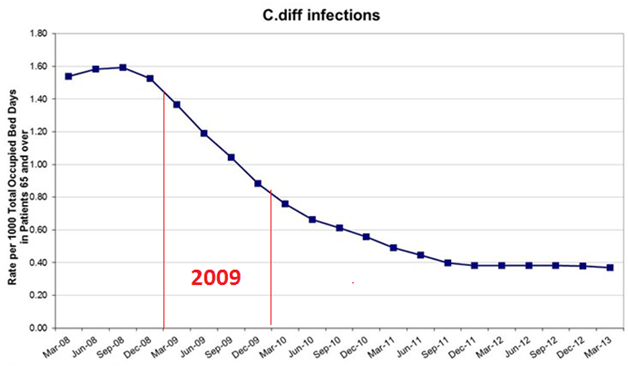
These fudged statistics are apparently the best evidence that Hygiene Solutions can produce to support their claimed Deprox performance, after the system has been in use for 8 years and in over 60 hospitals.
A Freedom of Information request¹ to UCLH disclosed the starting and finishing dates of their disastrous Deprox decontamination contract with Hygiene Solutions Ltd. The Deprox operations started in June 2013 and ran continuously, 7 days per week through to October 2016. The contract called for at least 4 Deprox units to be at the hospital, and 6 or more processes to be completed daily.
However, due to frequent breakdowns, Hygiene Solutions struggled to meet their obligations, and on occasion asked engineers to put a non-functional Deprox unit in a room, tape up the door and “run” a process – thus not only defrauding the NHS but leaving a dangerously contaminated room that the staff believed to have been sterilized.
Plotting the contract dates against the quarterly UCLH C. difficile data² (extended through 2016 with mandatory government reporting data)³ reveals an exact correlation between the period of Deprox deployment and a substantial step change in the number of C.difficile infections – approximately 70 extra cases over the 29 month period.
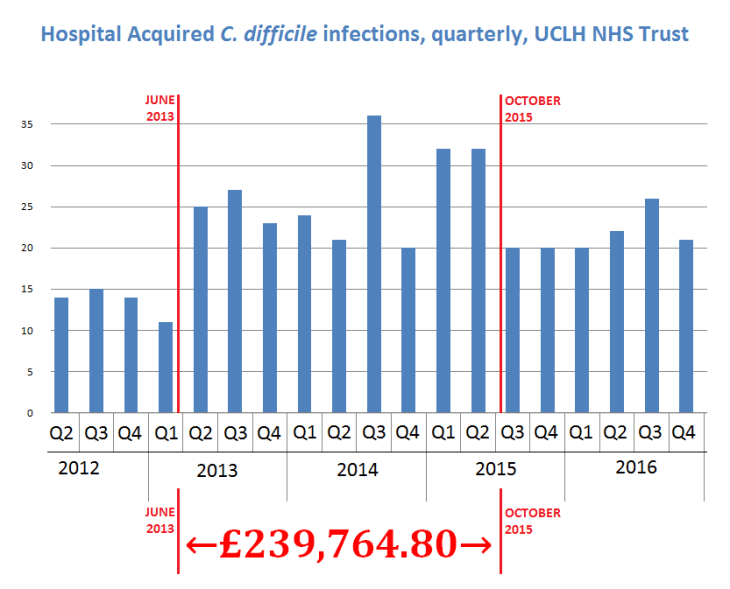
According to the March 2016 government report on C. difficile mortality, the 30 day mortality rates for the London area were about 17%. This would suggest that about 12 of these 100 extra infected patients would have died within 30 days of C. difficile diagnosis. Any patients who acquired C. difficile or any other Heathcare Associated Infection, (HAI) in the UCLH hospitals between June 2013 and October 2015 should consider contacting a medical negligence solicitor and seeking compensation.
[1] https://www.uclh.nhs.uk/aboutus/wwd/Annual%20reviews%20plans%20and%20reports%20archive/Infection%20Control%20Annual%20Report%202015-16.pdf (See graph, p.17)
[3] https://www.uclh.nhs.uk/aboutus/FOI/FOI%20disclosure%20list/FOI2017271Response.pdf
https://www.dropbox.com/s/71u3j3fcdqwqfnj/ResponseFOI2017271.xlsx%20%28~13%20KB%29.URL?dl=0