The emperor and all his barons then came to the hall; the swindlers held their arms up as if they held something in their hands and said: “These are the trousers!” “This is the coat!” and “Here is the cloak!” and so on. “They are all as light as a cobweb, and one must feel as if one had nothing at all upon the body; but that is just the beauty of them.”
“Indeed!” said all the courtiers; but they could not see anything, for there was nothing to be seen.
Hans Christian Andersen (1837)
“Marketing is what you do when your product is no good.“
Dr Edwin Land, inventor of the Polaroid camera

If a business is to sell its goods, it must persuade the customer that:
- The products will provide benefits proportionate to their cost.
- That they will do so more cost-effectively than competing products.
The customer then will weigh up the perceived benefits and costs of the products he is considering purchasing, and place his order accordingly. The key word here is “perceived”. The purchasing decision is based on the customer’s perception of the benefits of the product, which may differ from the reality.
Creating this perception is called “marketing” and as Edwin Land rather cynically pointed out, can be particularly helpful if your product is no good.
Hans Anderson takes this observation a little further – his famous tale, as well as entertaining children, makes the interesting point that if the marketing is sufficiently convincing and persuasive, the “product” can be dispensed with altogether, and the enterprising businessman can be handsomely remunerated for providing nothing at all. (At the risk of offending a minority of readers, I will point out homeopathic medicine as an excellent example of this phenomenon.)
Where the product or benefit does not actually exist, it is very helpful from a marketing perspective to have some visible and tangible “props” to induce the well known placebo effect. These can be as simple as “chalk pills” or as complex as large machines with sound effects, smoke, and flashing coloured lights. Hans Anderson was well aware of this:
“And he gave the swindlers a large sum of money, in advance, that they should set to work without any loss of time. They set up two looms, and pretended to be very hard at work…”
The deception is made immeasurably simpler if the “active ingredient” is invisible. (To sell “hypothetical” potatoes, for example would be problematic) Hence the plethora of therapeutic devices in the late 19th century based on the invisible phenomena of electricity, magnetism or (unfortunately) radioactivity. For example, we have:


We now leap forward a century or so to 2016. Medical technology has advanced beyond recognition, but the language of medical marketing seems strangely familiar:

The grammar may be unconventional, but surely this is not quackery? Medical sterilisers are tightly regulated by both European and UK standards and directives, and have to be tested on daily, weekly and annual schedules by trained and qualified personnel. Any deviation from a claimed efficacy would be immediately discovered.
Not so. Sterilisers and autoclaves for medical equipment are indeed highly regulated, but devices such as Deprox for sterilising and disinfecting hospital wards, intensive care units and operating theatres merely have to have a CE mark – they are classified as janitorial equipment, and the only regular testing they receive is an annual PAT test for electrical safety.
We have here the perfect opportunity to make large sums of money from nothing:
- A regulatory loophole.
- An invisible and odourless “product” (Hydrogen peroxide vapour)
- An invisible, but deadly problem (bacteria and viruses)
- Ineffective or overpriced competition (Glosair and Bioquell)
- A very obvious and public need for hospitals to slash the levels of “Healthcare Acquired Infections” (HAIs)
A carcase of this size soon draws the vultures,* and Specialist Hygiene Solutions Ltd. of King’s Lynn have not been behind in their attentions. With commendable diligence, they are ingesting in the order of 3 to 5 million pounds per year of the NHS budget.
What does the NHS get in return for this weighty expenditure? Nothing?
No – worse than nothing. The Deprox process not only fails utterly in the task it is intended for, it is also detrimental, harmful and potentially lethal to vulnerable patients in NHS care.
Extraordinary claims require extraordinary proof, and that is what I will attempt to give.
The Deprox fraud began in a very specific time and place – Room A16-K11, Tergooi Hospital, Blaricum, The Netherlands, 27th June 2007.
Here is the scene:

On the left is the IC-4 hydrogen peroxide decontamination unit, designed and built by Infection Control BV in the Netherlands. On the bed is an array of bacteria cultures in petri dishes. Each dish contains 1,000,000 bacteria or bacterial spores, and there are a variety of different substrates in different dishes. These samples are called BIs (Biological Indicators) The temperature is 250 C, relative humidity 38%, and the machine is set to atomise a 5% hydrogen peroxide solution until the relative humidity is increased by 40% (ΔRH40). The room size is 3.5 x 5m (about 10’ x 15’) and has a volume of 49m3. Once the door has been closed and sealed with tape, the machine will start and run for a two hour test cycle. The test is being conducted by TNO Built Environment and Geosciences, a large international architectural and construction consultancy.
When the machine starts, a white fog blows gently upwards from the two chimneys of the IC-4, and being dense and cold with evaporation settles down around the machine like a slow-motion fountain. In time, as the air is repeatedly circulated through the machine, the room becomes filled with mist.
Once the two hours is up, according to the test report, the following procedure takes place:

The reasons for these precautions become clear when we look at the following graph.
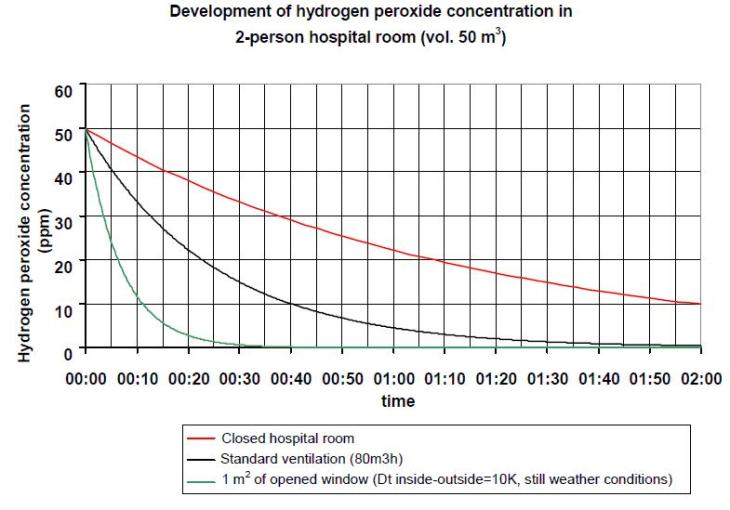
This shows the change in H2O2 concentration in the air once the IC-4 machine has finished the decontamination stage. The safe level of H2O2 for human exposure is 1ppm. If the room remains sealed at the end of the process, the H2O2 is still at 10ppm after 2 hours. By wearing goggles, holding his breath, rushing in and opening a window and rushing out again, supervised by a colleague in case he loses consciousness, the operator can have the room safe to re-enter in 30 minutes.
The samples are now removed and incubated to determine the efficacy of the process. If a particular sample proves to be sterile, i.e. all 1,000,000 bacteria are dead, this is called a log6 or 6log10 efficacy.
The results of this test along with a number of other tests and assessments of other aspects of the IC-4 process are contained in TNO Report 2007-D-R0951/B “Disinfection using Hydrogen Peroxide”. As most of the biological indicators in the June 27th test were sterilised, the report came to the following conclusion:

The TNO report is long, poorly organised and difficult to interpret, but is essentially factual. It is misleading in the sense that for the efficacy test described the BIs (pathogen samples) were all laid out in a horizontal plane, facing upwards, within 2.5m of the machine. (TNO report, p16) The fog settles preferentially on horizontal, upward facing surfaces close to the machine, producing a visible film of moisture, and leaving a visible silver nitrate deposit. Other surfaces in the room remain dry. The test samples clearly were not representative of surfaces in other orientations and more distant locations.
This is confirmed by a similar test reported in a paper by Beswick et al. in 2011.
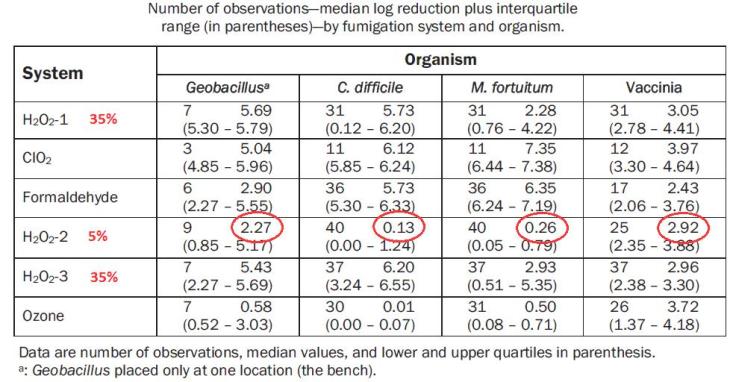
The room disinfection systems tested included a 5% H2O2 fogging system (row H2O2-2 in the table) similar to the IC-4, and gave log 2-3 efficacy. For this test, in a similar sized room, most of the samples were placed in more sheltered locations such as under cupboards or inside an open centrifuge.
A 2013 paper; The inactivation of Bacillus subtilis spores at low concentrations of hydrogen peroxide vapour.(D.J. Malik et al.) summed up test data from their own and previous tests to give a formula for the from which the efficacy of any concentration of H2O2 vapour against bacterial spores could be evaluated. The graph below shows that 50ppm (which is the average aerial concentration for the IC-4 test) gives a very low log reduction against B. subtilis spores.
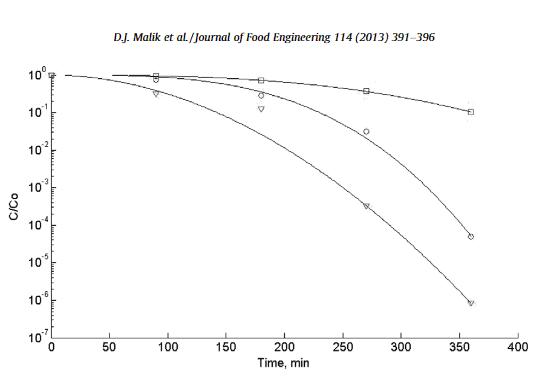
Fig. 2. B. subtilis spore inactivation data (solid lines are data fits using Weibull regression model), squares (50 ppm); circles (75 ppm); triangles (90 ppm).
Numerous other papers give results for fogging systems based on 5% H2O2 solution, with efficacies ranging from log0.1 to log4. No papers report log5 or log6 efficacy for any 5% H2O2 system against any pathogen. It seems reasonable to assume that the sterilisation of the log6 BIs in the TNO test was due to droplets of solution falling on to the samples, then both the H2O2 and silver nitrate becoming concentrated as the samples dried after the test.
In about 2009, Rick Fentiman a young and very ambitious entrepreneur founded Specialist Hygiene Solutions. Rick had considerable business and marketing flair, but no medical or scientific qualifications beyond A level (He claims to be a Cambridge University graduate microbiologist – but isn’t). Initially Hygiene Solutions were just the UK agents for Infection Control BV, and used the IC-4.
The IC4 sold very well in the UK, and Infection Control BV were unable to build the machines fast enough to keep up with the demand. Rick then bought the rights to the IC-4 design from Infection Control, and reverse engineered it in to a more streamlined product, called Deprox.
Hygiene Solutions retained the IC-4 on their website until mid 2016, even though the Deprox had long since superseded it. This was because the IC-4 was, in their words “the patented technology base for the Deprox process” What this actually meant was that they had utterly failed to achieve any useful efficacy whatever with the new Deprox, so had to rely on the original IC-4 data to “validate” their log6 claim, see below:
Please see Appendix 1, the “TNO Report” which validates the efficacy of the IC4™, the patented technology base to the Deprox system. This testing set out to evaluate the efficacy achieved by the Deprox technology on an extensive range of surfaces, positions and angles to best replicate the typical busy hospital environment.
(Sheffield Teaching Hospitals Response to Tender, 2014)
We will assume for the moment that the IC-4 genuinely did demonstrate a log6 efficacy. Is it honest for Hygiene Solutions to claim this performance for their re-engineered Deprox machine?
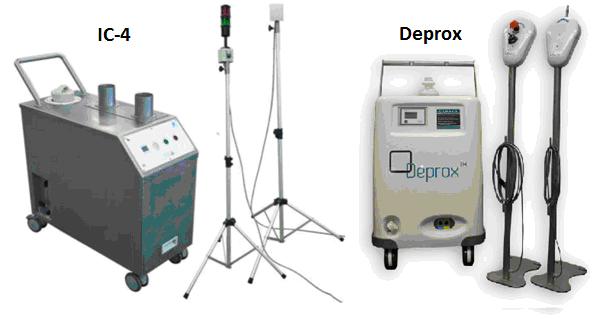
Here we need to consider how these machines work. Examination of the patents of each machine shows that they have the same internal equipment and components, the only significant difference being the orientation of the inlet fan. So far, so good. On these criteria the IC-4 tests do indeed seem relevant the Deprox log6 claim.
But what about the other variables – process time, room size, and the settings that govern the concentration of H2O2 attained? We need to look in more detail as to how the process is controlled:
From the Deprox patent:

The “RH difference above the ambient” is called ΔRH (i.e. change in Relative Humidity) This rise in humidity is caused by the water in the H2O2 solution evaporating. As the ratio of water to H2O2 in the solution is fixed, the ΔRH setting is roughly proportional to the H2O2 concentration that the machine achieves.
Changing the ΔRH setting changes the efficacy of the process. The efficacy is proportional to the H2O2 concentration, which is in turn proportional to the ΔRH setting.
The IC-4 tested in the TNO report was set to ΔRH40. This worked well for the test, but proved impractical for real hospital applications for two reasons:
- If the initial humidity of the room was over 60%, the process would fail as the dew point would be reached before the atomisation finished.
- The H2O2 concentration at the end of the process was around 50ppm, and would take several hours to reduce to a safe level. Obviously the method used in the test of “hold your breath and open a window” was impractical and dangerous.
There are obvious technical fixes for both these problems, which could easily have been incorporated in the new Deprox – a dehumidifier, to dry the air before the process starts, and a catalyst to remove the H2O2 at the end of the process. Humidifiers and catalysts are expensive, however, and Hygiene Solutions wanted to keep the Deprox as cheap and simple as possible. With a flash of true genius, the directors of Hygiene Solutions realised that both problems could simply be solved by turning down the ΔRH from 40 to 20.
So the Deprox differs from the IC-4, in that it delivers approximately half the concentration of H2O2 and hence has a greatly reduced efficacy. No problem – both the gas and the germs are invisible, so no one will know. As long as the “log6” claim is trumpeted loudly and clearly, that is what the customers will believe that they get.
Having so successfully applied the Hans Anderson principle to this first problem, the Kings Lynn prodigies eagerly searched for other aspects that could benefit from this treatment. The Tergooi tests were done in a small, 2 bed room of only 49m3. However, the majority of bed space in UK hospitals is in the form of traditional large wards with 4 or 6 bed side bays and in many cases a larger 8 to 12 bed bay at the end of the ward, up to 380m3 in volume or roughly 8 times larger than the test room.
From a marketing perspective, to have a machine that could decontaminate a 12 bed bay in a single operation would be a great advantage – competing systems such as Glosair would require 2 or 3 machines operating simultaneously. If a single Deprox could only be made powerful enough to decontaminate such large rooms, the competition would be finished.
The conventional approach to achieving this would be to start with a research and development project, involving real scientists and measurements and other inconveniences. Hygiene Solutions has no time for such things. (Of course, their Technical Director is sometimes a “Cambridge University Graduate Microbiologist”, but only for marketing purposes.) In the clear light of their personal post-scientific dawn, the directors saw that they need only pretend that the Deprox had this capability. By simply saying that the Deprox could give a log6 reduction over the whole 380m3, magically, it was so. (After all, no one was likely to enter the room during a process, and wander around with a hydrogen peroxide meter). Thus we have:
Each Deprox system can treat up to 380m3 (Sheffield Teaching Hospitals Response to Tender, 2014)
“…the swindlers held their arms up as if they held something in their hands and said: “These are the trousers!”
What is the real performance of a Deprox likely to be in a 380m3 12 bed ward?
The Deprox draws air through its atomiser unit at a rate of 2m3/minute, so in the 90 minute decontamination phase it will have circulated about 180m3. So even in ideal conditions, less than half of the air will pass through the machine.
Unlike the IC-4, the Deprox air intake is on the bottom face of the machine. In operation the weak column of cold vapour is ejected vertically, and typically collapses before reaching the ceiling, falling down around the machine and then being sucked in again. The Deprox thus creates a small convection cell around itself, leaving the rest of the air in the room still and undisturbed. This has serious consequences, as follows:
After one or two passes, air entering the atomisation chamber is fully saturated, preventing the droplets from evaporating and releasing their H2O2. Effective operation would require dry air to pass through the chamber. The poor design and weak fan of the Deprox ensures that the same small volume of air passes through the chamber multiple times.
Outside of the convection cell, there is no air movement, as the room is sealed and the ventilation turned off. The only mechanism to distribute the H2O2 around the room is diffusion, which is a slow process. To illustrate this, the smell of coffee brewing doesn’t instantly spread through a large room, and in still air may take several minutes to be discernible from a distance. Even then there is a gradient – the concentration is stronger closer to the source.
With hydrogen peroxide there is an additional factor – the gas is unstable in air, breaking down spontaneously in to oxygen and water. From the graph in the TNO report we can see that this decay is in the order of 20% over a 15 minute period.
Like a leaky bucket, the further the H2O2 is carried, the less of it there is. (This problem can be very simply solved by using a couple of oscillating fans – but why complicate matters – the gas is invisible, after all)
The result of this combination of factors is a very inhomogeneous distribution of H2O2 around the room. This is explored in detail by the TNO report – the graph below illustrates the effect.
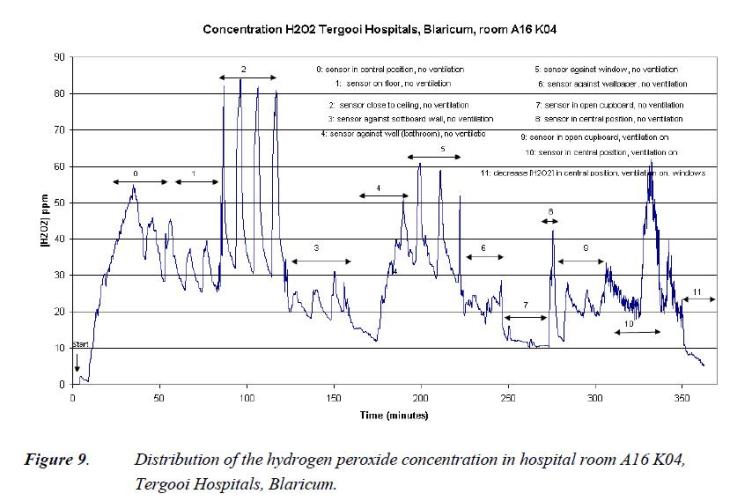
Here the researcher, presumably wearing breathing apparatus, has moved the H2O2 sensor to different locations in a 92m3 room during an IC-4 process. The very large variation is obvious. In a 380m3 room, the inhomogeneity will be proportionately worse. In addition, sheltered locations such as the inside of an open cupboard (7.) have well below the average H2O2 concentration.
Is this a problem? – no, this is merely a fact. Hygiene Solutions is never deterred by facts. Nurses and microbiologists in hospitals are deeply worried by the corners and crevices that pathogens can lurk in, inaccessible to disinfectant wipes. True to its name Hygiene Solutions has a solution – they will pretend that the Deprox can disinfect the insides of cupboards, and any other confined space, including complex equipment!
The areas that have been hard to disinfect in a room are treated to the same high standard with the DEPROX including behind the radiator, the underneath of tables, inside lockers, the small crevices and complex equipment.
(Royal Marsden Proposal 2015)
“Indeed!” said all the courtiers; but they could not see anything, for there was nothing to be seen.”
Now the hardworking NHS nurses and domestic staff can sleep soundly at night. Every crack and crevice has been rigorously sterilised, and their precious patients are safe. What an amazing advance in disinfection technology!
Now to revisit the question of whether the IC-4 test result is applicable to Deprox.
The IC-4 apparently demonstrated a log6 efficacy in the following conditions:
- A 49m3
- Samples horizontal, facing upward, lying on the bed adjacent to the machine.
- ΔRH setting of 40%
- Four specific test organisms, all bacterial.
Based solely on this one test, and with no additional or upgraded capabilities whatever, the Deprox is claimed to demonstrate a log6 efficacy in these conditions:
- A 380m3
- Pathogens inside lockers, on the underside of tables and in small crevices.
- ΔRH setting of 20%
- A “broad spectrum of pathogens” “Even the most virulent of organisms”
In other words, they have taken the IC-4, halved the output, multiplied the room size by 7.6 and claim that not only will a log6 efficacy still be attained on flat, horizontal exposed surfaces but also in small crevices etc.
This seems very damning. The reader may hope that this is the end of the story, but no – to quote from the Sheffield Tender submission,
“With a continual dedication to reaching beyond what we have already achieved, our technology never stands still.”
Hygiene Solutions did indeed reach beyond what was already a remarkably bold, shameless and criminal deception. At the end of 2014, they made it worse by a factor of 4. The Marketing Manager, Mark Fentiman sent an email to the service department instructing that the entire fleet of Deprox machines were to be turned down from ΔRH20 to ΔRH5.

 The logic behind this rather drastic decision is as follows:
The logic behind this rather drastic decision is as follows:
A H2O2 decontamination system has two main tasks;
- To put enough gas in to the air to kill the germs.
- To get the gas out again, so humans can safely enter
H2O2 is unstable in air, and in time breaks down completely. At the 50ppm level that the IC-4 achieves, about 4 hours would be needed for the gas to break down naturally to a level where the room was safe to enter. Time is a scarce luxury in NHS hospitals – there is constant pressure to make beds available for new patients, and even a few hours set aside for decontamination puts an immense strain on the system. A rapid process time is thus a good marketing point, and a way to get ahead of the competition.
In order for the total process time to equal or better the competing systems, Hygiene Solutions needed to reduce the “deactivation phase” to just 45 minutes. The output had already been turned down by 50%, which had reduced the deactivation time to about 1.5 hours but this was still too long to wait.
A catalyst could be used – Hygiene Solutions had even prototyped and tested one, but the active material, palladium, was costly.**
There was a better solution – H2O2 is practically odourless – so why not just pretend that after 45 minutes the room is safe to enter?
Hence we get:
-
With an integrated deactivation system, the Deprox completes the entire decontamination process and subsequent deactivation with a single unit.
(This is an imaginary deactivation system. It had no physical manifestation at all. It is a “prop” to the 45 minute deactivation illusion, but a virtual prop, not a real one.)
-
With the real-time monitoring function of the Process Analyser, the Deprox system is intelligent as to concentrations of hydrogen peroxide in the treatment environment
(As for item one. Doesn’t exist. Sounds good though.)
-
…it will only display a green light on the remote Process Monitor when ambient conditions have reached levels within the EU regulatory exposure levels.
(Hygiene Solutions have dug deep in to their pockets and installed no less than 9 green lights (real ones) to clearly prove that the room is safe to enter.)

It isn’t safe – H2O2 levels are likely to be 5 or 6 times the legal limit – but most people don’t notice, and look how much time it saves!
(Presumably if Hygiene Solutions designed pedestrian crossings, the lights would be green for both cars and pedestrians simultaneously. We would all appreciate the saving in time, and we could pretend that children didn’t get run over.)
Unfortunately for Hygiene Solutions, some nit-picking customers became concerned about symptoms of watering eyes and burning throat, when re-entering a room after a process. At least one healthcare cleaner experienced long term respiratory illness, see doctor’s letter below.
Instead of reporting to the Deprox manufacturer for warm words of reassurance, these customers used a H2O2 meter and found the H2O2 levels to be way over the limit, in spite of the generous array of green LEDs. Pretending that the room was safe just didn’t work when the customer would insist on checking.

After much thought and deep consideration, the wise directors came up with a radical and very original solution. They would simply turn down the output of the machine to such a low level that there was no H2O2 left for the imaginary deactivator to virtually deactivate, or for the pretend H2O2 sensor to pretend to sense! So they quietly, and without any hint to the customers turned down the whole fleet of machines to ΔRH5.
The shocking fact is that Hygiene Solutions continued to provide their Deprox systems and “decontamination” service at this dangerous and utterly ineffective level, did not inform their 60 or so NHS Hospital customers of the change, and continued to charge full price, a tidy sum of £2,500,000 per year.
We can see from the graph below the effect of this decision. The efficacy of a disinfection process is proportional to the area under the graph, i.e. the concentration multiplied by the time. The yellow block represents a 90 minute process at 170ppm, which according to the research of D J Malik et al. is the level required to give a log6 efficacy against bacterial spores. The orange area is the graph from the TNO test of the IC-4 at ΔRH40. The small blue area is the result from testing a Deprox at ΔRH5.
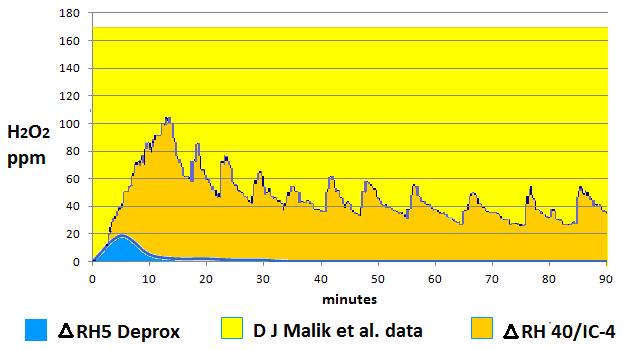
Broadly speaking then, Malik et al. suggest a concentration x time of 15,300ppm minutes to achieve log 6. The IC-4 gave 4500, about 30% of Malik’s figure. The Deprox at ΔRH5 gave about 100 i.e. 2.2% of the IC-4 output, or 0.73% of the theoretical concentration x time required.
The reason for this disproportionately large reduction is easy to see. The Deprox only gives a single pulse, then stops atomising for the rest of the 90 minute period. This is because the Deprox monitors the RH, and allows it to drop by a pre-programmed amount before triggering a second pulse. A large initial rise in humidity as given by the IC-4 will fall equally rapidly, as absorbent materials in the room quickly adjust their humidity to come to equilibrium with the new, much higher humidity of the air. However a small rise of 5% as given by the Deprox produces a much slower absorption, and the RH level remains almost constant for so long that a second pulse is never triggered.
Our updated IC-4/Deprox comparison becomes:
| Process | Output ppm x time as % of log6 Malik data | Room size
(m3) |
Sample environment |
| IC-4 | 30 | 49 | Exposed facing up |
| Deprox | 2.2 | 380 | Any, including crevices |
As mentioned before, the rain of droplets on the samples in the TNO test is the most likely cause of the log6 reduction measured. However, in the small test room the IC-4 did hold the average concentration at the equilibrium figure of 50ppm for the whole process, so probably gave a similar performance to the Glosair machine and other 5% aerosol processes, i.e. around log2 or log3.
What then is the likely performance of the Deprox? It is running at just 2.2% of the IC-4 output, yet must fill a room 7.6 x greater in volume. Quite simply the Deprox is doing NOTHING AT ALL. No measurable level of disinfection could possibly result from this process. It has simply become a prop, like the swindlers’ looms. The machine hums and whirrs, coloured lights flash red, then finally green and the process is complete.
Given that approximately 5000 NHS patients die each year from the very infections that this system is supposed to prevent, there can be no doubt that this action led to completely avoidable infections and death, as well as robbing the NHS of millions of pounds in fees for thousands of imaginary decontamination services that never actually took place.
Deprox® gives hospital staff the assurance that full decontamination has taken place and that the new patient is not at risk from cross-contamination.
From the process monitor located outside the room the operator is immediately aware when the bio-decontamination cycle is complete with a clearly visible GREEN light. This feedback mechanism ensures that rooms are quickly released for patient use as soon as they have been successfully bio-decontaminated, in other words…. “DEPROX’d”.
It should be noted that The Deprox instruction manual gives the first step in the decontamination process as
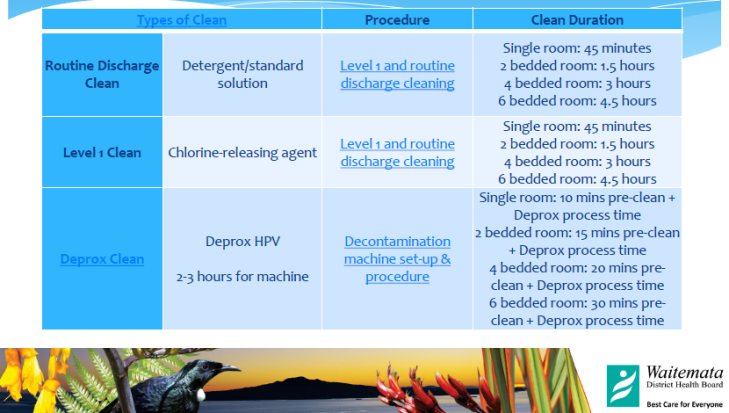
“Clean Room using manual cleaning methods and detergent and set up room for vaporisation process” (Royal North Shore Proposal 2012)
Clearly the Deprox process is not intended to be supplementary to conventional hospital “deep clean” processes such as hypochlorite disinfectants. It replaces them. Here the Deprox fraud becomes lethal – as dangerous in fact as the pathogens it falsely claims to kill.
From the North Shore Hospital, Waitemata DHB, New Zealand, we can see clearly that the Deprox is reserved for the most seriously contaminated rooms. It is also obvious that the Deprox’d rooms do not receive a conventional clean – they just have a “pre-clean” i.e removing soft furnishings, obvious gross decontamination etc. The level one chlorine based clean is obviously much more effective than a Deprox set at RH5. How many New Zealand patients have died as a result of this shocking fact one can only try to guess…
From the Hygiene Solutions website we find the following data, intended to promote their product:

As Hygiene Solutions rightly say:
When decontaminating a room in preparation for the next patient, it is essential to deliver the highest log reduction available in order to thoroughly decontaminate the environment. This is fundamental in reducing hospital acquired infections.
Every year over a thousand patients in NHS hospitals die of Healthcare Acquired Infections such as C. difficile and MRSA. The front line of defence against HAIs is manual deep cleaning with strong disinfectants such as hypochlorite. Hygiene Solutions has displaced these powerful cleaning methods, and substituted a fake and completely ineffective placebo that leaves rooms, operating theatres and equipment contaminated and dangerously infectious.
According to Hygiene Solutions;
The DEPROX delivers a particularly significant contribution to society because, as it is so effective in killing C. Diff spores, it actually saves a significant amount of lives each year.
Consider that there are around 160 Deprox units “working” every day in 60 NHS hospitals around the UK. It is inevitable that a number of patients have died and many more have suffered from entirely preventable infections as a direct consequence of the Deprox process.

Death squad: Deprox units lined up at a UK hospital
* The reader may find this analogy between Hygiene Solutions and vultures rather harsh and unfair. I would somewhat agree, and offer an unreserved apology to any vultures who may have been offended by the comparison.
** Hygiene Solutions did subsequently retrofit a catalytic deactivator to the Deprox – the problem with the ΔRH5 setting being that the machines hardly used any of the Deproxin solution, which was a major source of revenue. Once the machines were all upgraded , they were reset to the default ΔRH15. However, after a few weeks the catalysts became ineffective, almost certainly because the palladium granules get coated with silver nitrate from the Deproxin fog. So at the time of writing, Hygiene Solutions are in the process of turning the machines down to ΔRH5 again, starting with those hospitals that use H2O2 detectors for example the Leeds Teaching Hospitals Trust .